I am a Certified Pump Trainer (CPT) for all 5 pumps currently available on the market. I have been doing insulin pump therapy trainings for almost 2 years now. The number of patients using insulin pumps is growing rapidly. If the patient is motivated and willing to take on some additional responsibility for their diabetes care, an insulin pump could be a useful option. I do insulin pump demos and patients usually chose between 2 or 3 of the 5 pumps. I realize this is a big personal decision to make, and of course insulin pump therapy is not the right decision for everyone.
Patients should select a pump that would best suit their lifestyle and easiest for them to use. The physician should not be the one choosing their pump. How does it work? Once the patient makes a choice, the insurance verification is started with the pump company and they get in touch with the patient. I have no contact with them until the patient receives the pump and calls me to schedule the training. I then provide instructions prior to the training. I think it is very important that patients request to be educated by a Certified Diabetes Educator who specializes on Insulin pump therapy. Please note that the Eisenhower Diabetes Program does not sell or promote any particular pump.
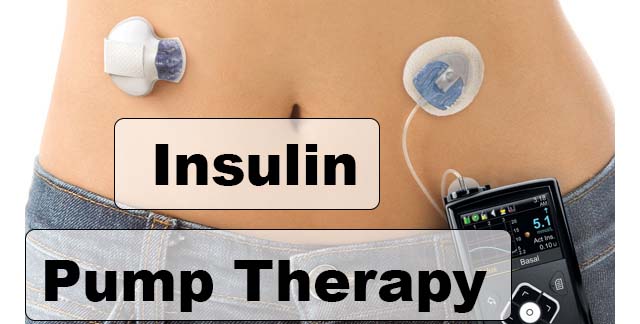
How Insulin Pump Therapy Works
Insulin Pumps are small devices that are battery operated or charged with a cable just like you would charge a cell phone. Insulin pump therapy consists of a pump, a reservoir, an infusion set which is a catheter that is inserted in the fat under the skin in the abdominal area, the tight, or arms. The site needs to be changed every two-three days. The reservoir t is filled with the amount of rapid-acting insulin needed for 2-3 days. The plastic tubing that is primed with insulin connects the pump to the person’s body. Delivering the insulin continuously with the pump closely imitates the action of our healthy, working pancreas. Insulin pumps are external, and can be discreet. They are usually either in a pocket, clipped to a belt, or hidden within your clothes. Depending on the brand and model, they hold between 180 and 315 units of insulin. The programmed rates are determined by your healthcare professional. Settings needed are basal rate which is the amount of insulin continuously delivered for 24 hours and bolus dose which is an on demand delivery to match carbohydrates and to correct the sugar if already high. Some of the pumps also have the Continuous Glucose Monitor integrated (CGM) and that helps to see their glucose every 5 minutes on the pump screen. The patient has to insert a sensor and add a transmitter to be able to transmit glucose levels directly to the pump via infrared or radio waves. With this new technology, there is less glucose testing but is not replaced.
For more informative articles read the following:
How to use Insulin Pump Therapy
The insulin pump must be programmed with the basal rate, a user’s insulin sensitivity factor, insulin-to-carbohydrate ratios and glucose target. Basal rates are delivered continuously for 24 hours 7 days a week. The correction or sensitivity dose is how much one unit of insulin decreases glucose points and the carbohydrate ratio is how many grams of carbohydrates are covered with one unit of insulin. The person wearing the pump has to check the glucose before each meal and enter the result in the pump. The user must still count the grams of carbohydrates that would be consumed at the meal and enter them in the pump to receive insulin coverage. In order to be able to make any changes on the pump settings if the patient states that their glucose is too low or too high, it is important that the patient enters the glucose and carbohydrates into the pump to see if the settings are correct or need to be adjusted.
Insulin Pump Therapy in Patients Undergoing Surgery How it Works?
People on insulin pumps can still keep their pump at the discretion of the anesthesiologist or surgeon if they are having minor surgery that would last less than two hours. If having major surgery, the pump needs to be removed and insulin must be given intravenously. Also, since the person would be NPO (nothing by mouth after midnight) the basal rate on the pump may need to be decreased the night before. It is important to monitor more often for hypoglycemia. If you are doing okay after surgery or admission to the hospital, you can keep the pump with agreement of the hospital team.
Insulin Pump Therapy with Automated Insulin Suspension
There is a pump that currently has a threshold suspend. This means that a sensor inserted just under the skin, reads glucose every 5 minutes and transmits it directly to the pump. The pump stops delivering insulin for two hours if glucose levels fall below patient’s lowest glucose target unless the person can acknowledge that they are okay and resume insulin delivery immediately. In a way that is good, if the patient’s glucose is low and can lose consciousness. However, if the patient’s glucose is normal and the sensor sends a false low glucose level to the pump and it stops the insulin, the person can end up with very high blood sugar if they don’t resume the insulin right away. A problem I have found with some patients often on this particular pump due to sometimes the inaccuracy of the sensor.
What is U-500?
HUMULIN® R U-500 is concentrated human insulin indicated to improve glycemic control in adults and children with diabetes requiring more than 200 units of insulin per day. U-500 is five times more concentrated than regular insulin and it is for people that have very high insulin resistance due to obesity. U-500 can be used with the insulin pumps, but close monitoring is recommended to prevent severe hypoglycemia episodes. The U-500 insulin is for people with type 2 diabetes who have not met the glycemic control goals with regular intensive insulin therapy.
Is there an Insulin Pump with no Tubing?
The Omni Pod pump is the only one that is tubeless and disposable. The PDM (Personal Diabetes Manager) controller is the meter to check glucose and the remote to the pump. The pod holds 200 units of insulin. The cost of the Omni Pod System is less expensive initially ($800 PDM versus $6,000 pump) but the overall cost is comparable during a three years to four years period. The big attraction for most is the lack of tubing that allows for more freedom and they are less likely to become disconnected.
Can I Gain Weight or Lose Weight on this Therapy?
It depends. Insulin pumps do not cause weight gain with a healthy diet and exercise. Having a pump doesn’t mean that a person can eat anything they want whenever they want. Insulin pumps actually limit excess weight gain. Eating habits improve as patients don’t have to overeat when treating hypoglycemia. Which is what often happens when patients have low glucose, and they tend to over treat and they gain weight. Also, having the CGM can help see how foods affect their sugar and help make diet changes. Better weight control is another potential benefit of using an insulin pump.
How Much Does an Insulin Pump Cost?
Insulin pumps can cost between $4,500 and $6,500 for individuals without insurance. The price varies depending upon the features, brand and the pump. You still may have to pay a monthly fee for your supplies depending on your insurance coverage. Insulin pumps are usually covered by most private insurance companies under the durable medical equipment of your policy. You must read over your paperwork carefully as often times it’s quite difficult to find the true answer. You may have to pay a deductible and/or coinsurance unless you have met the yearly out of pocket maximum.
How Does an Insulin Pump Attached to the Body?
The infusion set consists of tubing that connects the reservoir in the pump to a cannula (tiny tube to deliver insulin subcutaneously placed in the fat under the skin) and transports the insulin from the pump to the person’s body. The pump’s tubing is attached to the insertion site on the body.
How can an Insulin Pump Help a Person with Diabetes?
An insulin pump can help people to take the insulin subcutaneously and not have to do multiple daily injections anymore. Other potential benefits are: less frequent severe hypoglycemia, improve glucose control, reduction of hemoglobin A1c and better quality of life.
Is Doing Insulin Pump Therapy Okay for People With Type 2 Diabetes?
Yes, some public health and private insurance plans will only pay for a specific pump. There are general eligibility requirements if you want to be put on insulin pump therapy. People with Type 2 diabetes should be receiving at least 4 daily insulin injections per days, other possible criteria for an insulin pump is if you are having frequent hypoglycemia while on insulin, have advanced complications of diabetes, or frequently have high blood sugar.
Insulin Pump Therapy Side Effects
Adverse issues are usually associated with user error and not from a pump malfunction. Sometimes there may be an issue with a site reaction. Improper site selection, inadequate pump education and lack of support may be contributing factors of adverse events.
What are Insulin Pump Therapy Advantages and Disadvantages?
There are many more advantages than disadvantages for insulin pump therapy
Advantages |
Disadvantages |
|---|---|
|
|
Is an Insulin Pump Right for Me? How do I Know it is Right for Me?
If you or a person that has diabetes and uses insulin, an insulin pump might be the right choice. Ask your diabetes educator to tell you about what features might be best for your needs. Insulin pumps are a long term decision, and it’s normal to rely on a pump for 4 to 5 years, so it’s important to discuss different options with your health care provider so that you can assess the features and choose a pump that is right for you.
Insulin pumps are not for everybody. Not all patients with Type 2 diabetes are recommended to use an insulin pump, especially if the diabetes is already under control using oral medications. They are also not recommended for patients with pre-diabetes. It’s best to speak to your physician about whether you should use an insulin pump or not.
Is an Insulin Pump Covered by Medicare?
Yes, government insurances such as Medicare Part B and Medical cover external insulin pumps and the insulin the pump uses under durable medical equipment for people who meet certain conditions. A patient's out-of-pocket cost under government insurance varies depending on the policy.
Is an Insulin Pump Permanent?
No, the pump is not permanent. You have the freedom to disconnect from the pump for swimming, showering, or anything else that may get on the way with the pump such as intimacy or sports. Try not to be disconnected for more than 30-60 minutes at the time though, to prevent Diabetic Ketoacidosis, DKA. Check your sugar if disconnected longer than 30-60 minutes.
Further reading:
What is the Most Common Risk of Insulin Pump Therapy?
There is risk for Diabetic Ketoacidosis (DKA) from the pump malfunctioning, running out of insulin, dead battery, occlusions or absorption problems. DKA is a serious condition that can be fatal. DKA happens when there is not enough insulin in the system and sugar gets too high. There are alarms set up on the pump to go off if sugar gets too high or too low or if there is no insulin delivery. All those potential problems should be addressed during the training.
Hypoglycemia is also another risk if the person is not eating for long periods of time or is more active than usual. Never forget that the pump is delivering insulin continuously 24/7. Otherwise the pump settings can be adjusted to fit your life style.
If you have any comments post them down below!
TheDiabetesCouncil Article | Reviewed by Dr. Christine Traxler MD on June 05, 2020





