Have you ever stood in the middle of a see-saw, right over the center with one foot on each side? Trying hard not to put more weight on one side to keep it stable? Unless you are incredibly focused, it can be very difficult to keep a proper balance without one side touching the ground.
The struggle is similar when trying to balance two medical conditions, such as diabetes and celiac disease. While each one has specific needs, they both need to stay balanced which can be hard to achieve.
This article explains celiac disease and its relationship with diabetes.
Contents
What is celiac disease?
It's a condition where the body recognizes gluten, a protein found in some foods, as a poison. The body tries to attack it to prevent it from being digested and entering into the bloodstream. When someone with celiac eats gluten (which is found in foods that are made with rye, wheat, or barley), the small intestines react by changing the lining. Normally, there are long, fingerlike structures that line our intestines that absorb the nutrients in the food that we eat. With celiac disease, those finger-like structures become flat to protect the body from absorbing the gluten. Additionally, the gut stops making digestive enzymes, to also prevent from any absorption. The image below gives a good illustration of what happens in the small intestines when gluten is eaten.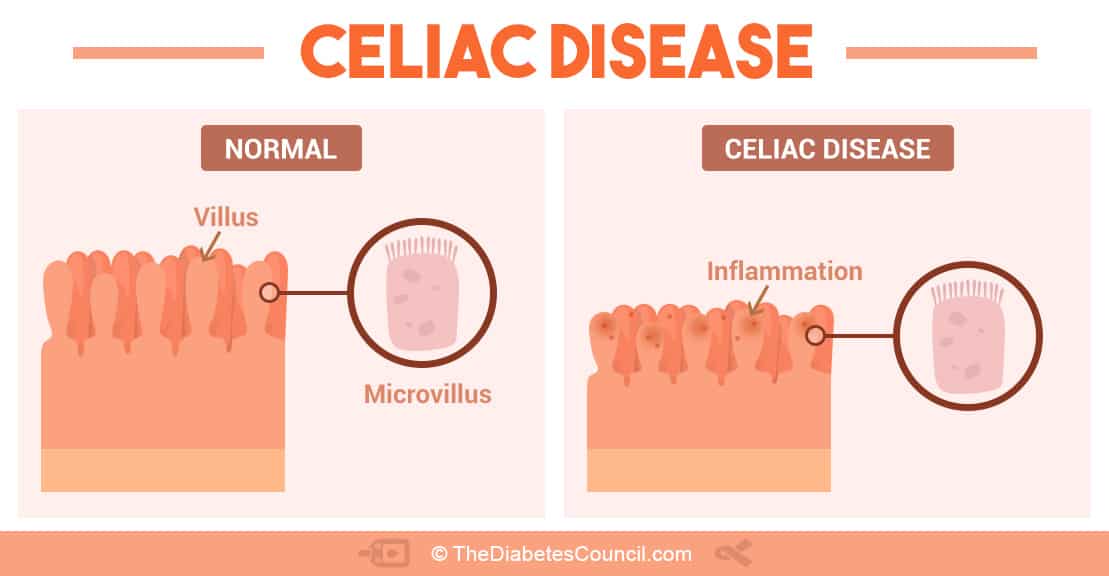
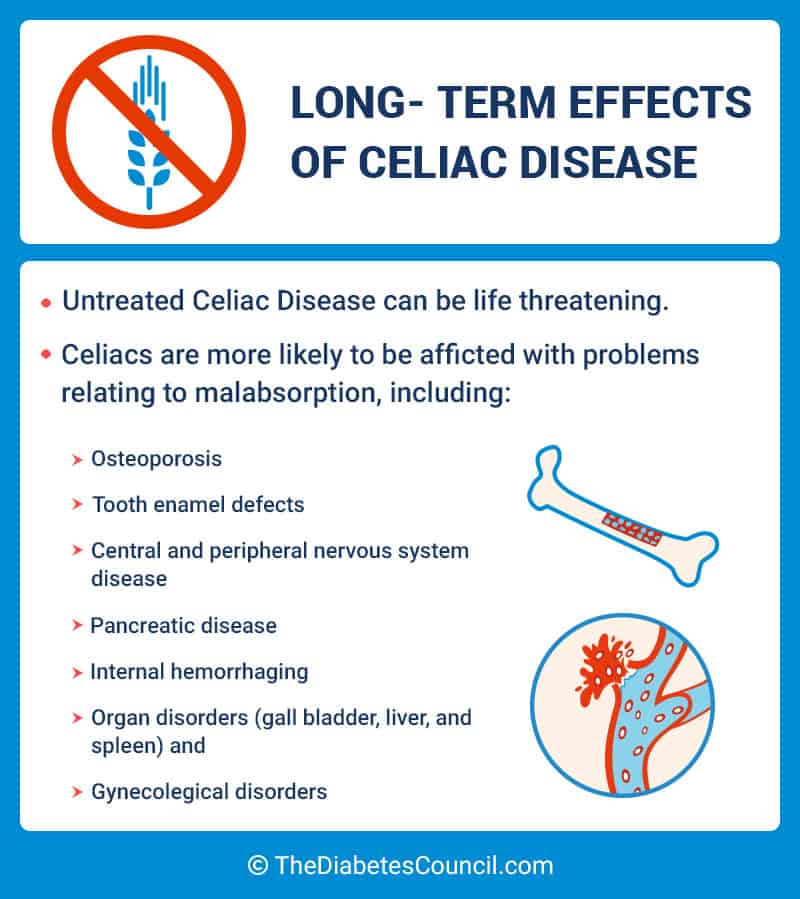
The problem with this is that over time, it permanently damages the small intestines and prevents nutrients and vitamins from being absorbed. Long-term malabsorption can cause issues such as:
- Osteoporosis
- Anemia
- Infertility
- Organ disorders
- Delayed puberty
- Stunted growth
- Inability to gain weight
- Weak tooth enamel
- Seizures
- Depression
Currently, 1 in 133 healthy people have celiac disease, and that number seems to be increasing. Because of this rise, it is vital that people are aware and educate themselves about the disease so they can seek treatment sooner and stop the long-term complications.
I advise reading the following articles:
So what is the treatment?
It is to simply eliminate gluten from the diet.
How do I know if I have it?
Most people with celiac disease do not show symptoms; therefore they are not fully aware that they have it. There are certain risk factors and symptoms that can initiate testing from your physician.
If you have any of the following risk factors or symptoms as discussed below, you should talk to your doctor about screening.
Risk Factors
One study found that possibly 95% of people did not have any symptoms of the disease. If no signs are detected, it is then very important to look at risk factors as reasons to screen. Risk factors include: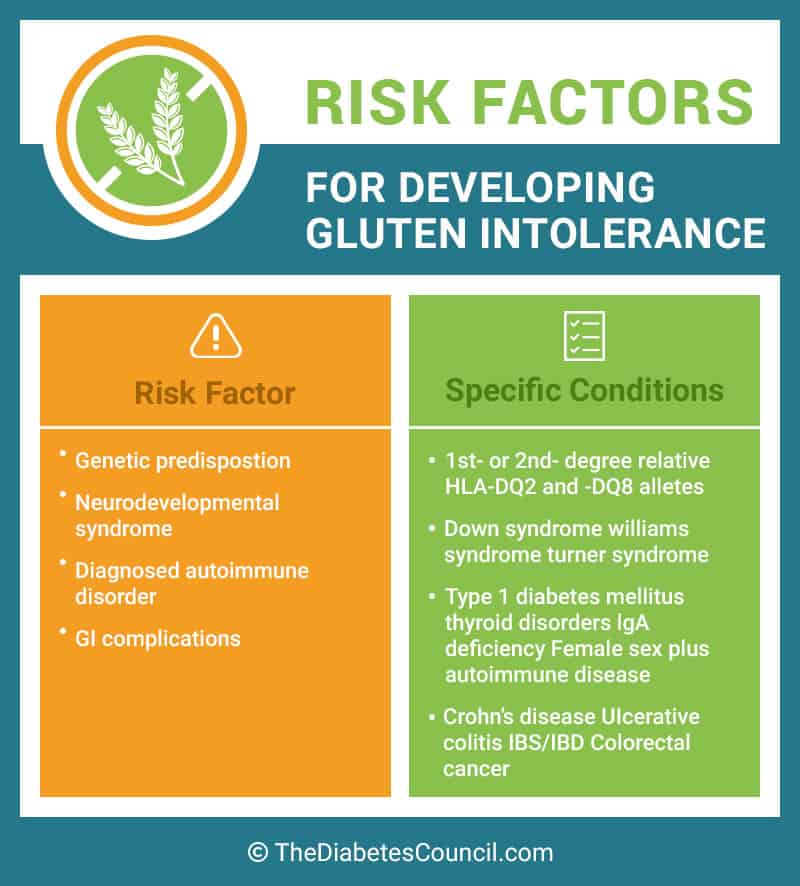
- Other autoimmune disorders
- Irritable Bowel Syndrome
- Type 1 Diabetes
- Having a relative with the disease (A 1 in 22 chance if an immediate family member has it!)
- Neuropathy
- Thyroid disease
- Down syndrome
- Female gender (2x as likely as males!)
- European decent (Italy actually screens all children under the age of 6!)
Signs and symptoms
There are over 300 signs and symptoms. Some people show none of them, while others have multiple. Several of the long-term complications, which can also be symptoms were mentioned above. Other, more acute indicators include:
- Gas
- Abdominal pain
- Canker sores
- Diarrhea
- Constipation
- Cramps
- Nausea
- Indigestion
- Foul smelling stool
- Bloating
- Memory problems
- Hair loss
- Anxiety
- Low blood sugar
Another symptom of celiac disease is a rash known as Dermatitis Herpetiformis. This itchy rash is commonly found on elbows, knees, buttocks, or back, but can be anywhere on the body. The following image shows a great picture of what the rash looks like.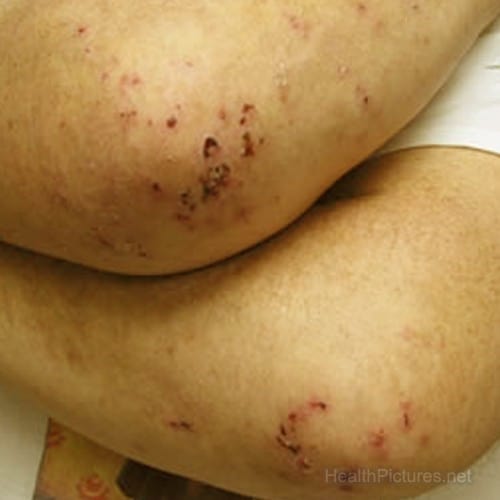
For an awesome website with information on symptoms as well as risk factors, check out https://www.beyondceliac.org/celiac-disease/symptoms-checklist. This interactive website lets you answer the questions and print out a sheet to take to your physician.
Testing & diagnosis
The simplest way to test is to do a blood test that checks for certain antibodies. Since celiac disease is an autoimmune disease, antibodies appear in the blood stream when the small intestines are attacking the gluten. However, the only definite way to diagnose someone is by doing an intestinal biopsy to see if there is any damage. Since this is pretty invasive, it is more difficult to do for everyone and the blood test is more common.
For people with risk factors for developing celiac disease or signs and symptoms, a screening should be done. Check out graph below and what it shows from a poll about screening.
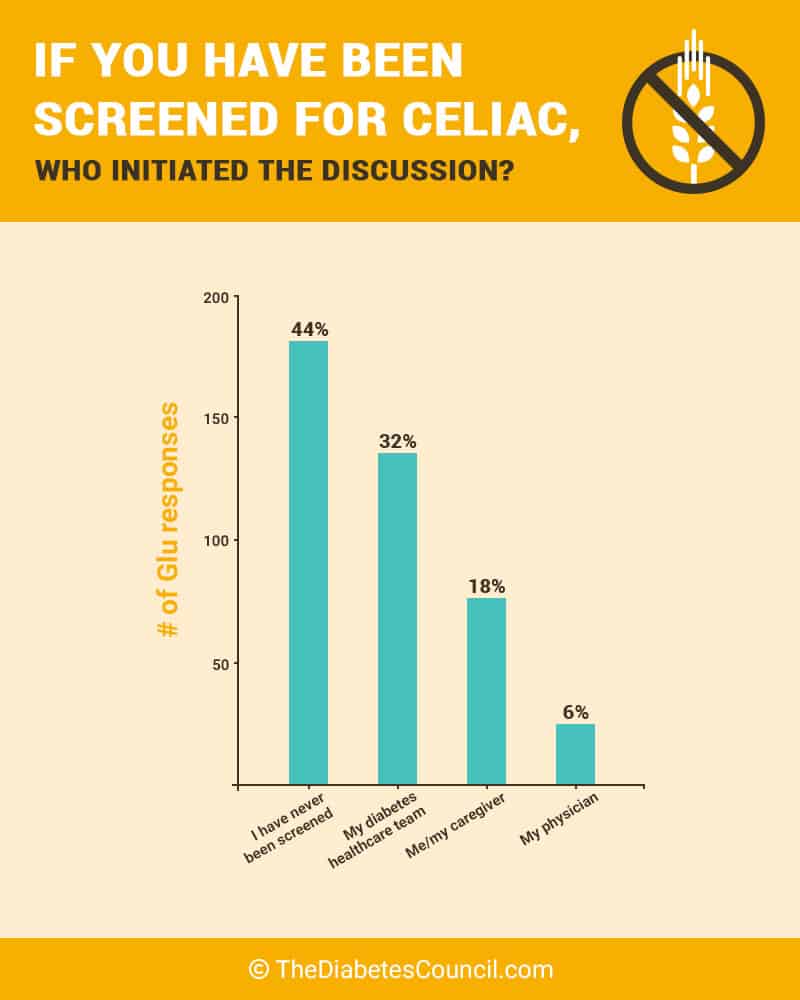
As you can see, it is not a common thing to test for and many people are not screened. It may be up to you as the patient to initiate it with your doctor if you do believe that you have the disease.
One important thing to mention is that if you are going to be tested, DO NOT stop eating gluten until after the testing is complete. If you do, your body will not produce the antibodies that the tests are looking for and it may come back negative! (How frustrating!)
Is it the same as gluten intolerance?
A gluten intolerance is a sensitivity to any foods that contain gluten. After eating gluten, a person develops mainly the stomach issues that are associated with celiac disease. (Bloating, abdominal pain, diarrhea, constipation, or cramping). The difference is that their small intestine doesn’t attack itself like someone with celiac disease. It is still very uncomfortable, and the only treatment is to avoid eating any foods that contain gluten.
Prevention and treatment
The treatment for celiac is pretty black and white. It is to completely eliminate all gluten from the diet. Sounds pretty simple right? Then why are only 78% of people with celiac disease complaint with their diet restrictions? It is because there are several foods (and non-food items) that contain gluten. Look at the following list to see some of them:

Fortunately, when gluten is no longer in the diet, symptoms can go away within a few days. However, it can take months to years for the intestines to completely heal. Any trace of gluten that is introduced into the body can create an autoimmune response that causes damage, and then the healing process begins all over again. For this reason it is very important for people to avoid any type of gluten consumption.
Cross contamination (when gluten-free food comes in contact with food containing gluten) can happen very easily. Toasters can hold crumbs from bread that can attach to a gluten-free piece of bread. Also, cooking utensils should not be shared from gluten containing dishes and gluten-free dishes.
For some, a gluten-free diet alone does not stop problems from occurring. Medications such as steroids and immunosuppressant drugs can be used to stop the body from destroying itself.
Celiac disease and Type 1 Diabetes
As I mentioned in the beginning of this article, there is a link between Type 1 Diabetes and celiac disease. 10% of people with Type 1 Diabetes have celiac disease. In the general population, only 1% of people have it. This is most likely because of the fact that they are both autoimmune disorders, and when you have one, you are more prone to have multiple.
Since some cases show no symptoms, it is important that all people with Type 1 Diabetes be screened for celiac disease to prevent the long-term complications. One study showed that after one year of a gluten-free diet, a group of children with Type 1 Diabetes and celiac disease had an increase in growth and a decrease in their A1C (a blood test that is done that takes an average of blood sugars over a 3 month period).
Having the disease is a problem for individuals with Type 1 Diabetes for a few reasons including:
- Balancing the diet is difficult
- Blood sugar levels are hard to control
- Dealing with both diseases can be stressful and lead to depression
Neither disease causes the other. Generally Type 1 Diabetes is diagnosed first because people show symptoms and the test is as easy as a blood sugar level. Lucky for them, that usually gives time to have a good understanding on the diabetic diet and recognize what foods they should eat and which ones they should stay away from. This is good because if they are diagnosed with celiac disease later on, they have established one of their diets already.
Type 2 Diabetes
Unlike Type 1 Diabetes, Type 2 Diabetes and celiac disease do not have a relationship. Type 2 Diabetes is not an autoimmune disease and is caused by hereditary and environmental factors such as obesity, poor diet choices, and a sedentary lifestyle. There are researchers, however, that believe that people with celiac disease are less likely to develop Type 2 Diabetes than the rest of the population. Some believe that this is because a gluten-free diet is lower in carbs (although not all foods as you will read soon!) which lowers the risk of Type 2 Diabetes. More studies need to be done before this is a proven fact.
Gestational Diabetes
There is no link between Gestational Diabetes and celiac disease. There is a chance that the stress and hormones can cause symptoms to worsen or appear for the first time for someone that already had the disease. With autoimmune disorders, stress can commonly trigger the disease or worsen it.
How does it affect blood sugar levels?
When someone with Type 1 Diabetes eats food and injects insulin, the sugar in the food pairs with the insulin for the body to use as fuel. With celiac disease, the small intestines do not allow for the food to be digested and the sugar molecules to be present. For those with both diabetes and celiac, the insulin doesn’t have anything to pair with and the blood sugar level drops.
For many people with Type 1 Diabetes, low blood sugar may be their only symptom. Low blood sugar is very dangerous because it can lead to problems such as seizures or loss of consciousness. If it becomes a common problem, schedule an appointment with your physician right away. Make sure you keep a log of the foods that you are eating as well as your blood sugar levels.
After beginning a gluten-free diet, a person with diabetes may discover that their blood sugar levels are increased. This is expected and should not be seen as a bad thing. It means that their body is finally digesting the food that they are eating and that the intestines are healing. Insulin or medication can be adjusted as needed after talking with the physician.
Back to the see-saw metaphor that I used in the beginning of this article: balancing both diseases can be very difficult because of how celiac disease affects the blood sugar. Many gluten-free versions of foods have different amounts of carbohydrates than their regular gluten-containing kinds. It is very important to read all labels carefully.
How to manage celiac disease and diabetes

Managing both diseases is difficult, but it is possible.
Find a dietitian that is specialized in both. They can identify foods that are beneficial for both conditions. It is important to note that one disease should not be considered more important than the other, so the diet needs to fit both of their requirements to avoid any complications. (Imagine the see-saw once again!)
Balancing your diet is a very important and difficult task. For example, a salad is an easy gluten-free meal. However, without proper amounts of carbohydrates and protein added to it, it can cause blood sugar to crash. Many gluten-free foods are low in vitamins, iron, protein, and fiber. It is very important to take a multivitamin to ensure you are getting all of the nutrients that you need.
What to eat and what not to eat
As previously mentioned, gluten is any food that contains barley, wheat, or rye. Some of the most common foods that contain gluten are pizzas, breads, crackers, cereal, gravy, and even beer. Also, there are many non-food items that contain gluten such as mouthwash, toothpaste, and even medications. Talk to a pharmacist about any medications that you are prescribed to verify that they are gluten-free.
Checking labels on food items is the best way to see if it does contain gluten. If there is a question, you can always contact the manufacturer and ask them. Remember that just a trace of gluten can make your body attack itself, so it is much better to be safe than sorry!
The following image is a list of some foods that are considered gluten-free. Read under each category about exceptions. For example, although fish may be okay, any breaded fish could contain gluten. Another example is yogurt. Typically it is okay, but some additives can contain gluten.
With the increase in the number of people with celiac disease in recent years, more brands are starting to make gluten-free versions of their products. As you can see from the image below, these items are clearly labeled and are specifically made for those with a gluten intolerance. Also, many restaurants have gluten-free options as well. When eating out, be sure to ask if the food prepared separately from the food containing gluten to prevent cross-contamination. Please be sure to check out our article on Gluten free diet and diabetes for more information.
Does eating a gluten-free diet affect blood sugar?
This question is very important for individuals with both diabetes and celiac disease. Many foods that are made gluten-free are higher in carbs and sugar to keep the consistency of gluten. This makes blood sugars increase and more medication or insulin may be needed. For example, look at the comparison in the image below of pancake mix that contains gluten (left) versus gluten-free (right). As you can see, the gluten-free mix has more total carbohydrates and sugar.
On the other end, some gluten-free items are made with substitutes that have less carbohydrates and sugar which can cause low blood sugar levels. A list of gluten-free flours that exist are listed below. As you can see, there are several of them. Reading the label for nutritional value very important. You need to know how many carbohydrates are in the product to properly dose insulin or medication.
If you want more information, www.celiac.org is a great resource. They have lots of gluten-free recipes as well as information about medications and other things that contain gluten. They also have a carbohydrate counter to help those with diabetes manage both of their diseases. Information on local support is listed for people who may need it. I highly recommend anyone to start there when looking for information and encouragement.
As most people with diabetes should know, carrying a snack around for hypoglycemic (low blood sugar) episodes is very important. For those with diabetes and celiac disease, carrying around the right snack is even more important. Gluten-free crackers or soybeans are great options for those moments that could become dangerous. Without the right snack, you could end up unconscious or grabbing a snack that contains gluten and causes your body to start attacking itself (not good!). Be prepared!
Are the signs and symptoms of celiac disease and diabetes the same?
Many of the symptoms of diabetes and celiac disease are similar (see the image below), however, remember that many people do not experience any symptoms and have silent damage occurring in the small intestines.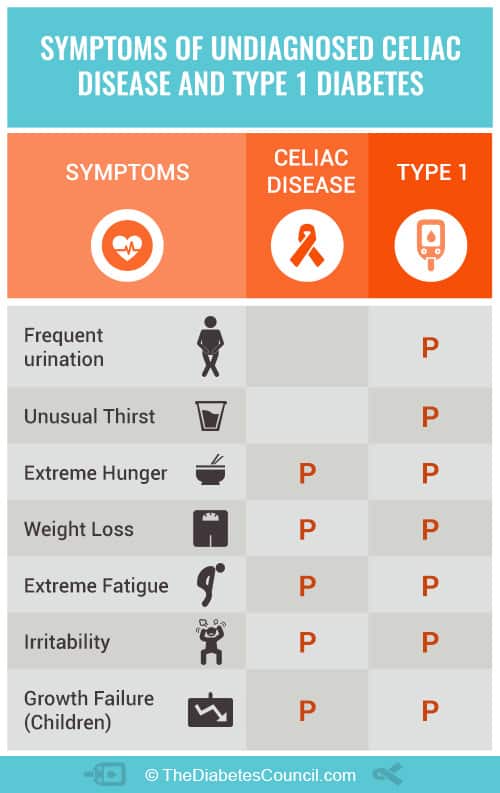
Because of these similarities, it makes it very difficult to diagnose celiac disease in someone that is already diagnosed with diabetes. This is another reason why all people with Type 1 Diabetes should be screened for it, regardless if they are showing any symptoms. Other issues that both diseases share include stomach problems and neuropathy (nerve damage).
Golden nuggets of knowledge
After all of this information, I want to summarize the important things listed in this article that I believe will have the biggest impact.
- If you have Type 1 Diabetes and you have not been screened for celiac disease, talk to your doctor about it. 10% of people with Type 1 Diabetes have celiac disease.
- Celiac disease, if untreated, can not only cause short term belly problems, but because none of the food is being digested it causes long term problems like osteoporosis, infertility, anemia, weak teeth, and neuropathy. (And this doesn’t even count the complications that diabetes can cause!)
- One disease does not take priority over the other. Talk to a dietitian that is specialized in both to give you support in making the best diet choices.
- Many gluten-free foods do not have the same carbohydrate and sugar contents as foods with gluten. When eating things, always read the label for the nutritional information to adjust insulin as needed.
- Find a support group to help you with dealing with both conditions. celiac.org is a great place to find lots of information as well as local support.
Can celiac disease lead to diabetes?
No, it cannot lead to diabetes. It is an autoimmune disorder, which is not caused by any specific thing.
Is a gluten-free diet good?
A gluten-free diet can be very good. When eating gluten-free versions of carbohydrates, the texture is different and takes some time to get used to. My daughter has a friend that has celiac and when she shares her gluten-free snacks, my daughter cannot tell a difference. Please read our article on Gluten free diet and diabetes.
Is it common in people with diabetes?
10% of those with Type 1 Diabetes also have it. This does make it common, since only 1% of the general population has it. It is not common for those with Type 2 Diabetes.
How does it affect diabetes?
Celiac disease affects diabetes by making it more difficult to keep the blood sugar in a good range. When someone with celiac disease is eating gluten, it can cause the blood sugar to be low because no food is being absorbed. Also, many gluten-free foods have different amounts of carbohydrates than foods with gluten, and that can make it hard to dose insulin.
Further reading:
Your thoughts
After reading this, it may seem overwhelming to think about all of the limitations and complications that these two diseases can cause. It may be difficult, but it is not impossible. Just like any other condition, having the right education and support can make a world of difference. Only 59% of people with Type 1 Diabetes and celiac disease follow the suggested dietary guidelines. This number is not as high as it needs to be. If you have any tips or insights on balancing both disease please share with others!
TheDiabetesCouncil Article | Reviewed by Dr. Christine Traxler MD on May 28, 2020
References
- https://celiac.org/celiac-disease/understanding-celiac-disease-2/celiac-disease-and-comorbid-conditions/cd-and-diabetes/
- https://celiac.org/blog/2015/08/celiac-disease-and-type-1-diabetes/
- http://www.beyondceliac.org/celiac-disease/related-conditions/type-1-diabetes/
- http://www.beyondceliac.org/celiac-disease/symptoms-checklist/
- http://spectrum.diabetesjournals.org/content/15/3/197
- https://www.gluten.org/resources/health-wellness/diabetes-and-celiac-disease/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3746085/
- http://www.diabetes.org/food-and-fitness/food/planning-meals/gluten-free-diets/
- http://www.medscape.com/viewarticle/747334
- https://www.celiac.com/gluten-free/topic/64591-celiac-and-hypoglycemia/





