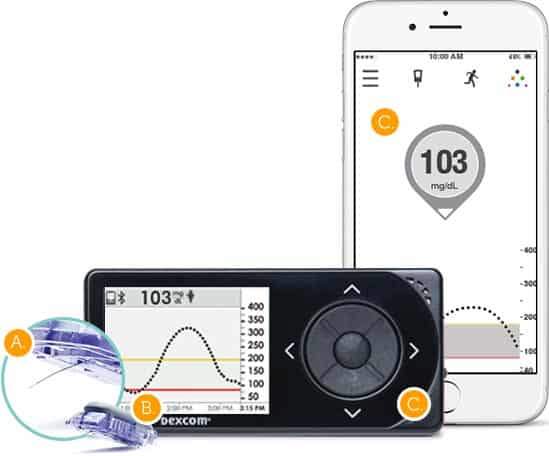
Source: https://www.dexcom.com/
You may find it hard to believe, but continuous glucose monitors have been around for quite a few years now. Almost all private insurance carriers are now covering them for patients with type 1 diabetes. There has been a battle amongst those advocating for better technology access for patients and the Centers for Medicare and Medicaid Services for almost 10 years now in terms of coverage for a CGM.
It’s an amazing step forward that those with diabetes are now living normal life expectancy. But the current coverage set up for those with diabetes in the Medicare system is limiting coverage on a lifesaving technology.
For younger patients with diabetes on commercial / private health insurance plans, tools like brand name glucose meters and strips, CGMs, and even insulin pumps are covered for the most part. The technology isn’t out of reach for a majority of individuals. What’s even better is when an insulin pump goes out of warranty a new one can be ordered every four years. There may be some variety in insurance coverage but a vast majority of patients have access to all these supplies and devices.
I recommend these articles:
Contents
Medicare is Different
In terms of coverage for insulin pumps, Medicare really makes patients jump through hoops before they will even consider it. They require that a patient undergoes a test to prove they are not making their own insulin and that they really need an insulin pump. Patients are not able to request one because they want to improve their management. Medicare will only pay for an insulin pump for individuals who quality every 5 years, so that means patients are spending one year using an insulin pump that is out of warranty. While this is a shocker, there are even limits on the types of pumps they will pay for.
Let’s Talk About Convenience

Medicare has adamantly refused in the past to cover CGM sensors, receivers and transmitters claiming they are simply “convenience items” and did not qualify for coverage. Additionally, the Centers for Medicare and Medicaid Services have stated that they do not meet the official definition of durable medical equipment, which keeps them falling under the DME category.
This is a tool that reduces the risk for people to experience low and high blood sugar levels as well as keep them from the emergency room or hospital, but it’s not deemed worthy of coverage. What is unfortunate is that those with diabetes could be using a CGM for many years then when they become of retirement age and have Medicare they no longer qualify. Hypoglycemic episodes are not just inconveniences to those who experience them, they are in fact a life-threatening condition that many people die from.
Prevention of Complications
You don’t have to be a brain surgeon to understand that the use of a CGM system could reduce medical costs for those with diabetes in the future. Learning how to detect high and low blood sugar levels before they occur can help prevent complications in the future. Keeping patients with diabetes out of the doctors’ offices and hospitals as they age from complications will save Medicare a great deal down the road.
Many advocates have stated that if Medicare would simply choose to cover the CGM technology that paying for the cost of CGM usage would cost the carrier much less than paying for frequent hospital admissions and ER visits. It’s unfortunate that the new technologies and advancing diabetes care treatments that are allowing patients to live a long sustaining life are not yet covered by Medicare.
It Takes a Community

The good news for many people on Medicare and those with Private insurers who use Medicare guidelines to determine coverage is that there are quite a few people on your side fighting the good fight. They are working diligently to get coverage of this technology for people with all types of diabetes. Petitions have been going around, many diabetes organizations have called to the masses of supporters to call their representatives to tell them that coverage of a CGM is lifesaving not just convenient for patients with diabetes.
It seemed that this path was a beaten road that wasn’t getting anywhere fast. The voices didn’t seem to make a difference, and Medicare was still refusing to coverage CGM technology for patients. That is until January 12, 2017 came around. This is a day that will live in the history books for those in the diabetes community.
A Monumental Decision
The Centers for Medicare and Medicaid Services made a determination that continuous glucose monitors would now be a durable medical equipment category that would be covered by Medicare. You heard right, the battle was won! All the hard work and determination paid off.
But now what does this mean moving forward?
This is a significant step towards making it so that CGMs are covered under Medicare. Extensive clinical data showed to key decision makers that CGMs helped to significantly improve diabetes management. This device allowed users to avoid low blood sugar episodes that could be potentially dangerous and even the long term effects of having elevated blood sugars. Senior citizens with diabetes are at a much higher risk of suffering a severe hypoglycemic episode, so the news of this potential coverage could be life changing for them.
Here's the Kicker….
In order for a CGM system to be included into the new category to qualify for Medicare Part B it must meet the definition of a therapeutic CGM which means it gives you the capabilities to make dosing decisions off of it. The only system right now on the market that falls into this category is the Dexcom G5 Mobile system.
Further reading:
The Debate Continues

Now that we’ve gotten past the Medicare debate of coverage, let’s discuss how CGM usage can help those with Type 2 diabetes better manage their condition. CGMs have shown to give promise to a better management routine of type 2 diabetes, but how it does it and for whom is still up for debate.
Many experts believe that CGMs can help to provide a layer of protection for patients who have Type 2 diabetes and are at a higher than normal risk for insulin induced hypoglycemia. Physicians believe that CGM usage should be on a case by case basis for type 2 patients. Those with normal a1c’s on metformin don’t necessarily need continuous coverage than a patient who’s had diabetes for many years now and requires insulin.
When these systems are used in type 2 patients they have been referred to as Professional CGMs. This is when the doctor applies the sensor and transmitter in the office and the user wears the device for up to 14 days to establish a pattern of blood sugars.
Wrap-Up
You can tell that this debate is one that has shattered the souls of those in the battle field many times when each time they’ve applied for this life changing and lifesaving technology, only to be denied. This endless cycle of denials seemed as if it would be never ending, but at last, a flag was planted and a new door to achieving coverage was opened.
Now a new battle lies, one that opens up all doors to this amazing technology for all people with diabetes not just type 1. This technology has proven countless times to be beneficial for everyone who has had the opportunity to try it.
TheDiabetesCouncil Article | Reviewed by Dr. Jerry Ramos MD on June 03, 2020




