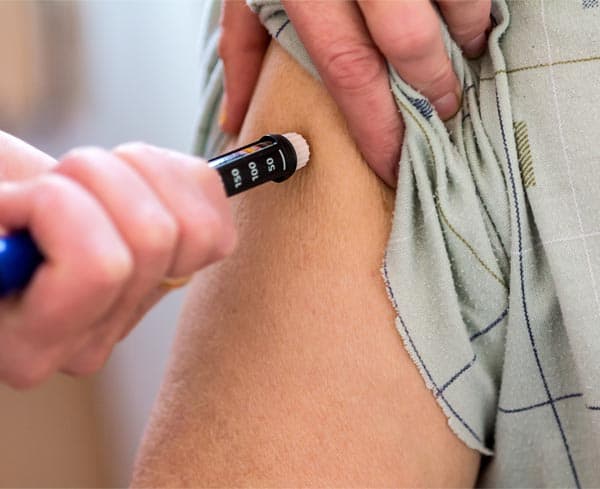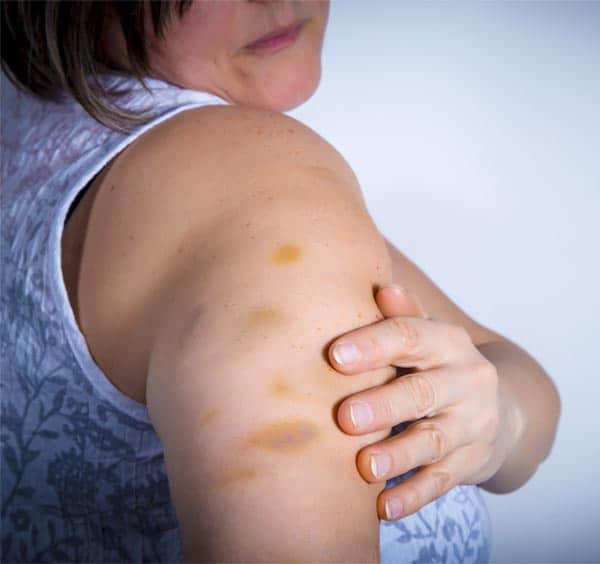
One common complaint you will hear from those with diabetes is about the amount of bruising that takes place from multiple injections.
While a bruise here or there seems like just something that comes along with injecting insulin, there are some things you can do to prevent frequent bruising from occurring.
While there are many reasons why you may experience bruising after an injection, you can try the following techniques to help reduce your chances of bruising.
- Ice the site where you will be giving an injection about 30 to 60 seconds before doing so. The cold temperature on your skin will help to shrink the capillary blood vessels which are more prone to getting punctured during an injection.
- If you notice that you experience bruising on your stomach more frequently ensure you are not injecting the insulin too close to your belly button. A good rule of thumb, or two fingers is to place two fingers around your belly button to get a general idea of how far two inches away will be. This is the suitable area that you can inject in.
- It may seem contradictory but the shorter your needles are the greater the chance you have at bruising.
- You want to inject your insulin at a 90-degree angle and not with a slanted angle. This will allow you to get into the skin easier and more efficiently than puncturing fully like the slanted angle.
- Rotating injection sites is extremely important as it can lead to bruising by using repeated areas. Scar tissue can also develop when you don’t rotate sites so this makes it more difficult for insulin to be readily absorbed into the body, allow it to not be used as efficiently as it should be.
Contents
Other Common Insulin Injection Issues
Bruising is not the only concern that those with diabetes have when it comes to injecting insulin.
In fact, there are many common issues that you can experience. If you are on multiple daily injections and have found yourself experiencing some issues, please read below to determine how to prevent these issues from occurring and how to handle them when they do.
I suggest reading the following articles:
Bleeding at Injection Site
It’s somewhat normal for a little bit of blood to appear when you do an injection. This is usually because the needle has punctured one of the tiny, capillary blood vessels under the skin. You can stop the bleeding when this occurs by putting a small amount of pressure on the site. Also, it’s important to:
- Never Rub the site
- If you do develop a bruise do not use this site again until the bruise has faded
- Keep light pressure on the site to try and prevent bruising
If you notice that you bleed quite frequently when you inject your insulin, you may not be injecting properly or may have an underlying issue. You should speak with your medical provider if this does occur.
Prevention of Pain with an Injection

- Wait until your alcohol swab has completely dried before you inject.
- Inject insulin when it’s at room temperature. Cold insulin can cause pain.
- Be sure to keep your muscles still and comfortable when injecting.
- Larger doses of insulin hurt than smaller doses.
- Don't reuse needles. Doing so can dull the tip and cause it to hurt more.
- Make sure you are not bending the needle when you remove its cap. The best method to remove the cap is to twist first then pull.
- Try not to inject into the muscle with a shorter needle such as an insulin pen. When you use needles that are 6m or longer you will want to pinch the skin up before injecting.
Insulin Leaking from the Needle after Injection
When you see this happen for the first time you may fear that you haven’t received your full dose of insulin. That’s not the case.
If it leaks after you remove it, you might just not be keeping the needle in the skin long enough. It’s a good idea to count to 10 before you remove the needle from the skin. Even after doing this, you may still notice a little bit of leaking after, this is normal. Before you remove the needle, try pinching up the skin as well to ensure the insulin goes directly into the skin and not out of the needle.
Outdated Beliefs and Myths in Regards to Injecting Insulin

Facts: Previously it was always a standard practice to pinch up a small layer of skin before injecting to avoid injecting into the muscle. Injecting into the muscle directly can hurt and it also increases your chance of developing hypoglycemia due to the faster absorption rate of insulin. But in days before when this was a common practice, the needles were much longer and wider. Today most needles are between 6 to 8 mm in length with pen needles being 4-5mm in length. Pinching for needles longer than 6 is important but with pen needles there is no need to pinch up. Pinching can also increase your risk of bruising.
Further reading:
Myth: You must always keep insulin in the fridge
Facts: Previously, this was true, but now when you open a vial or a pen cartridge it doesn’t have to be kept in the refrigerator. Cold insulin tends to hurt more when injecting so keeping it room temperature can help with this.
Unused insulin vials and cartridges should always be kept in the refrigerator to prevent it from being exposed to warm temperatures.
Injecting insulin isn’t something we’d necessarily want to do if we didn’t have to. But all you have to remember no matter the issues you run into, you are doing your very best and that’s all that matters. Speaking with your doctor or diabetes educator can help you to go over some concerns you may have when it comes to injecting insulin. Hopefully you don't bruise as easily with the help of this article, thanks for reading!
TheDiabetesCouncil Article | Reviewed by Dr. Christine Traxler MD on June 01, 2020