In this article we will cover everything you need to know about diabetes and your risk for Urinary Tract Infections. Do you have an increased risk of Urinary Tract Infections now that you have diabetes?
We will cover what a Urinary Tract Infection is, symptoms, diagnosis and treatment guidelines, as well as why they are more common in people with diabetes.
More importantly, we will discuss steps you can take to prevent them!
Contents
- What Is a Urinary Tract Infection (UTI)?
- What Are The Symptoms of a UTI?
- What Causes a Urinary Tract Infection?
- If You Have Diabetes, It Is Twice As Likely You Will Develop A UTI….Why?
- Can Diabetes Cause Frequent UTI’s?
- How Is A UTI Treated?
- Management of UTI’s with Diabetes
- How Does A UTI Affect Diabetes?
- Are Frequent UTI’s a Sign of Diabetes or Is A UTI a Symptom of Diabetes?
- How Can A UTI Be Prevented?
What Is a Urinary Tract Infection (UTI)?
A urinary tract infection or UTI is an infection anywhere in your bladder, kidneys or in the urinary system.
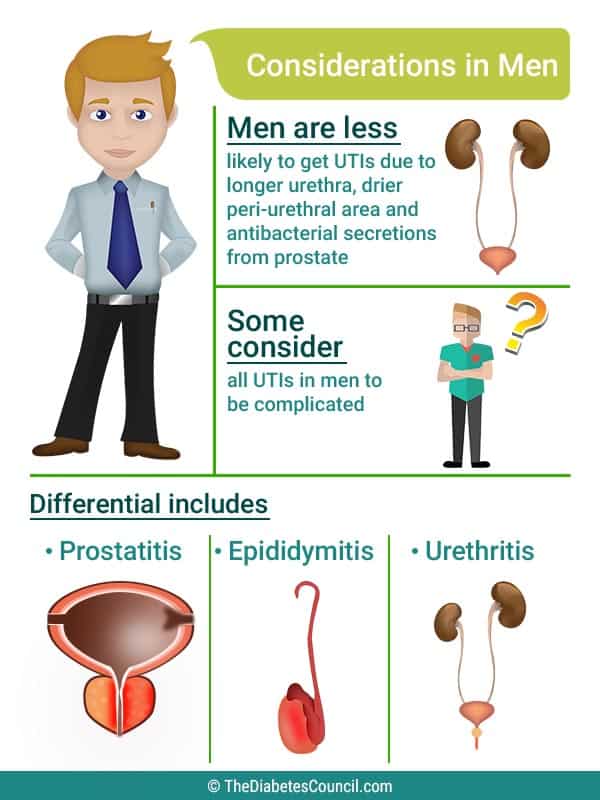
An infection of the upper urinary tract or the bladder is called a bladder infection or cystitis. An infection in the urethra is called urethritis. Women tend to be more at risk of these types of infections due to their anatomy; they have a much shorter area between the urethra and the opening to the urethra to the bladder. Urinary tract infections are rare in men under 50 due to their anatomy.
A more serious infection of the lower urinary tract is an infection of the kidney and the ureters and is called pyelonephritis. This is a complication and occurs when the bladder infection progresses to the kidneys.
I highly advise reading the following articles:
According to the Stanford Medicine’s Michael Hsieh Lab, half of women and men will have experienced a urinary tract infection (UTI) during our lifetime at least once. They are the most common infection, and can lead to death in patients who are experiencing it severely. Antibiotics are the most effective therapy.The National Institute of Diabetes and Digestive and Kidney Diseases account 8.1 million visits to the clinic, hospitals for UTI purposes. For women, the risk of getting a UTI is 50 percent greater than a man.
What Are The Symptoms of a UTI?
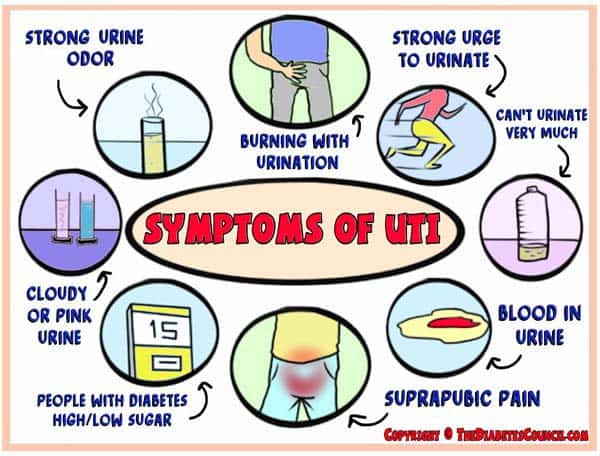
Let me just start by saying, if you have ever had a urinary tract infection, you certainly know the symptoms. They are not easily forgotten even if it has been years since your last one! Here is a list of the classic symptoms; some you may or may not experience:
- Burning with urination
- Strong urge to urinate
- Not being able to urinate very much at a time
- Blood in your urine
- Cloudy or pink urine
- Strong odor to the urine (learn more about what your urine is telling you)
- Suprapubic pain (pain near your pelvis)
- In people with diabetes: High or Low blood sugars
It is very important to note here that older people or people with autonomic neuropathy may not show any of the classic symptoms. The first symptom you may notice in an older person can be confusion and maybe a low grade fever.
In my years nursing, I have cared for so many elderly women who were unable to either feel the symptoms of their urinary tract infections or had dementia and were unable to communicate the symptoms to a caregiver. The first indication the caregiver had was worsening confusion and by then, the infection was severe enough to require hospitalization. Most of these patients also had diabetes, which put them at a much higher risk as well.
What Causes a Urinary Tract Infection?
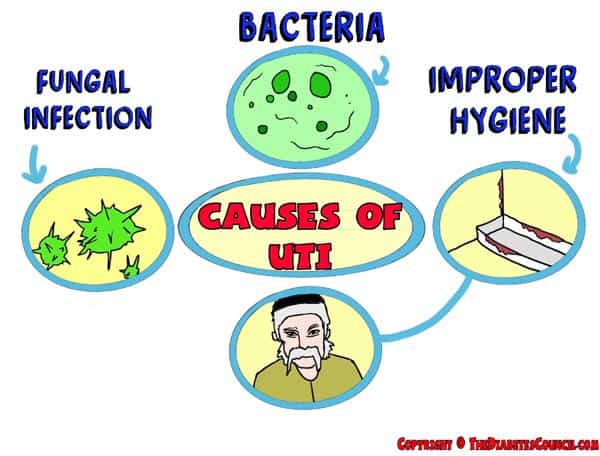
While the most common cause of a urinary tract infection is bacteria, it can also be caused by a fungal infection.
There are other several causes to urinary tract infections and for you, there could even be two things at once causing an infection! Unfortunately, improper hygiene can be the leading cause of urinary tract infections. Another leading cause, especially in people with diabetes and the elderly is urinary stasis or the bladder not fully emptying. Fungal urinary tract infections are an additional cause in people with diabetes, but happen less frequently.
If you have diabetes, chances are you have heard of neuropathy. Neuropathy is the damage that is caused to the nerves in your body from high blood sugars over time. Damage from neuropathy normally starts in your fingers and toes, and then moves to your hands and feet, on an upward spiral. This is called peripheral neuropathy; it continues moving upward until it reaches all of your body if you do not get your blood sugars under control while the damage is occurring.
For people with diabetes, autonomic neuropathy is a late complication of diabetes resulting in issues with the bladder and tracts within the bladder emptying properly. This leads to what is called urinary stasis, when urine is left in the bladder after you urinate. If the bladder does not empty fully, urine remains in the bladder causing bacteria to form, leading to the urinary tract infections.
This is why Certified Diabetes Educators are so concerned about trying to prevent complications related to diabetes; UTI is one of the complications. If you can’t feel your feet, you won’t feel a rock in your shoe. If you can’t feel that you haven’t fully emptied your bladder, you will begin to have many bladder infections.
Sadly, the complications of diabetes do get worse than this if your blood sugars remain uncontrolled. Not feeling your feet and experiencing frequent uti's are just the tip of the iceberg. That’s a whole other article though, but the bottom line here is, if your blood sugars are out of control for too long, get them in control quickly to avoid causing further permanent damage to your body! It’s all diabetes management and you can do this!
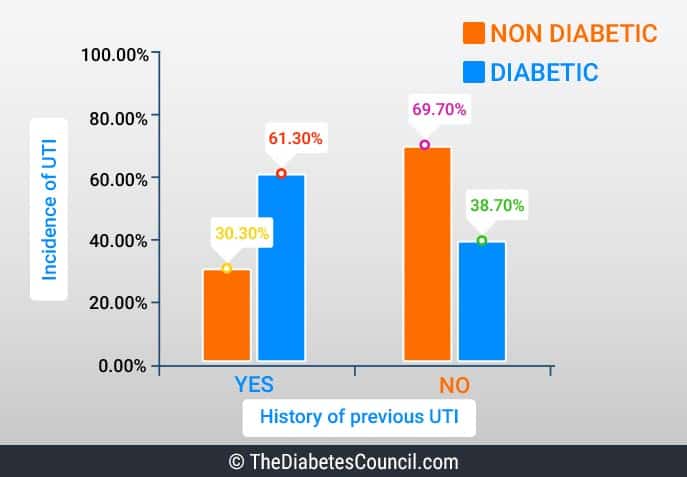
If You Have Diabetes, It Is Twice As Likely You Will Develop A UTI….Why?
There are many factors that elevate the risk for UTIs for people with diabetes. Common sense would tell us that higher blood sugars increase the risk for all infections.
Well, believe it or not, the jury is still out on that theory for some odd reason. I could not find any recent research anywhere on this theory or for that matter on urinary tract infections in people with diabetes. My hope is more research will be considered since the complications associated with these infections can be life threatening.
According to a study by Nitzan et al “Urinary tract infections in patients with type 2 diabetes mellitus: review of prevalence, diagnosis and management”, UTIs are most common and severe with complicated outcomes in people with type 2 diabetes. The study presents the reasons people with diabetes are at a greater risk for urinary tract infections which I will outline here:
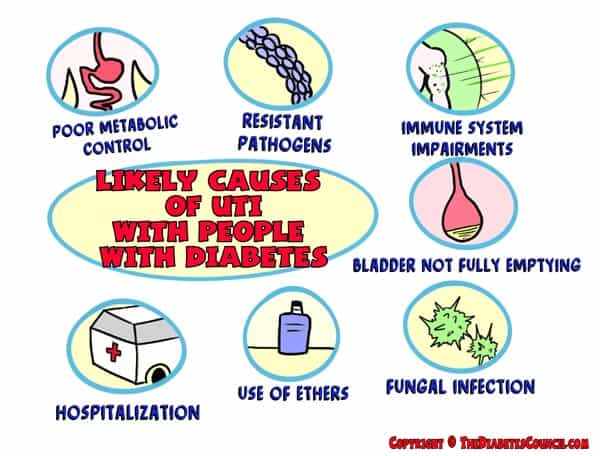
Likely Causes of Urinary Tract Infections in People with Diabetes:
- Poor metabolic control
- Resistant pathogens
- Immune system impairments
- Bladder not fully emptying
- Fungal UTI
- Use of catheters
- Hospitalizations
Poor metabolic control is not completely understood as a cause of utis yet, so this is a great opportunity for researchers. The extra “sugar” in the urine builds up, causing the growth of extra bacteria which leads to the infection in the bladder.
We have already discussed a few of these, but let’s discuss the ones we haven’t.
First off, resistant pathogens are bacteria that have become resistant to the drugs (antibiotics) we currently have to treat infections. This has occurred over the years for multiple reasons. One reason is people will get an infection, go to the doctor, get a prescription for an antibiotic for 10 days but only take 3 days of it, usually because they start feeling better. The infection mutates, they give this infection to another person and the cycle continues.
Now we are on the verge of superbugs that have evolved from this misuse of antibiotics. Healthcare professionals saw it coming and tried to warn about it years ago, but no one listened. This is already occurring now however, so I cannot stress strongly enough the importance of finishing a prescribed antibiotic for any infection to prevent infections from mutating.
People with poorly controlled diabetes are more prone to fungal infections. Fungus grows well in the presence of extra sugar. So again, if your blood sugars are high, you run the risk of a fungal urinary tract infection.
Hospitalizations can contribute to a higher risk of utis in everyone, due to the risk of contracting a hospital acquired UTI. Oh yes, you can catch everything in a hospital, even a bladder infection! This can be due to many reasons, but one is you may require a catheterization and that puts you at high risk. 40% of all infections caused in hospitals are due to indwelling catheters. The longer the catheter remains in place, the higher the risk. If you or someone you love needs an indwelling catheter while they are hospitalized, ensure the facility is following the current guidelines for changing the catheter. Also ensure the catheter is removed as quickly as possible. For men, external condom catheters are available as a safer alternative.
Can Diabetes Cause Frequent UTI’s?
The answer depends on your current level of control of your diabetes. People with poorly controlled diabetes may have more frequent utis due to the reasons already discussed. Getting your blood sugars under the best possible control will certainly reduce your risk of more frequent UTI’s.
How Is A UTI Treated?
The treatment for your uti will depend on what type of infection it is. If it is a bacterial infection, it will be treated with an antibiotic. If it is determined that it is a fungal infection, it will be treated with a different medication which targets fungal infections.
The first step your doctor will take will be to obtain a urine sample; this urine sample will determine if you have an infection. If so, the urine is then also cultured to determine which antibiotic it is sensitive to, in other words, which antibiotic will effectively treat and kill the bacteria. This will take a few days because the bacteria has to grow in a petri dish. See, there really are reasons some of these tests take time!
In the meantime, your physician will immediately start you on a broad spectrum antibiotic; this is an antibiotic that effectively treats many types of bacteria. If when the tests come back it is determined that you need a different antibiotic, your doctor will notify you and prescribe a different antibiotic which will treat your specific infection.
Sometimes the pain of a urinary tract infection is so great you may require a medication to alleviate the pain. Your doctor can prescribe a special medication which targets the pain associated with UTI’s.
Follow-up is essential to determine if the infection has cleared, so if your physician asks you to come back, please do so!
Management of UTI’s with Diabetes
Management of utis in people with diabetes is exactly the same, except you will be monitoring your blood sugars much more closely because you have an infection. As with any infection, we recommend that you check your blood sugar more frequently and contact the physician who manages your diabetes to let them know about your infection. You may need a temporary adjustment of your diabetes medications while you are sick.
If your blood sugars are very high, you run the risk of complications related to those high blood sugars even if you do not have Type 1 diabetes. Yes, people with Type 2 diabetes can be hospitalized for high blood sugars too!
If your blood sugar is over 250mg/dL this is considered too high and is at a dangerous level. Believe it or not, research shows you are actively doing damage to your body when your blood sugar is sustained at 150mg/dL 24 hours per day. Please contact your physician if your blood sugars start to rise if you get a UTI.
How Does A UTI Affect Diabetes?
Well, just like with any infection, a uti may cause your blood sugars to go higher. In some people, infections cause their blood sugars to go lower though. It varies from person to person, but most often, people will have higher blood sugars with an infection.
If your blood sugar begins to rise for no apparent reason, especially over the course of several days, I always tell my patients to suspect some type of infection.
Are Frequent UTI’s a Sign of Diabetes or Is A UTI a Symptom of Diabetes?
A review from 2005 found that an astounding 50% of people with diabetes have some type of dysfunction of their bladder- that’s half of every man and woman with diabetes. There are quite a few theories which we have already discussed, but again, most of the newer theories and research have only been conducted on rats.
Another fact this review highlights is that women who have Type 1 diabetes have a higher risk for kidney infections (pyelonephritis), which can potentially damage the kidney’s function long term. This may lead to the need for a kidney transplant as the damage becomes severe.
How Can A UTI Be Prevented?
Amanda recently contacted TheDiabetesCouncil asking how to prevent utis. There are quite a few simple things you can start doing today, that will ensure you don’t end up with another dreaded infection tomorrow!
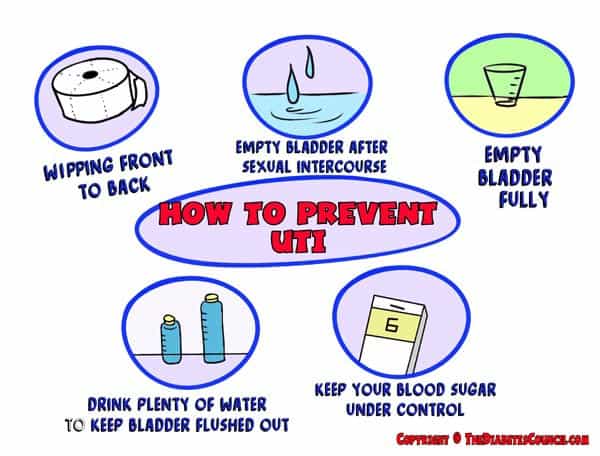
The very best prevention is to practice good hygiene techniques. Now remember, I am a Registered Nurse, so I am going to get technical here ladies:
- Wiping front to back is essential! Transfer of bacteria is definitely going to happen otherwise and will cause a urinary tract infection for sure!
- Go to the bathroom and empty your bladder immediately after sexual intercourse ladies.
- Every time you empty your bladder, try to make sure it is fully empty.
- Drink lots of water to keep your bladder flushed out; current recommendation is 8 eight ounce glasses per day (consult your doctor about how much water you should drink every day since people with kidney disease or other health issues may be on a fluid restriction).
- Keep your diabetes under the best possible control!
I know these techniques seem simple at first glance, but if you are vigilant, they really will work. Practicing these preventive techniques will go a long way in helping you stay healthy and hopefully avoid a potentially life threatening urinary tract infection.
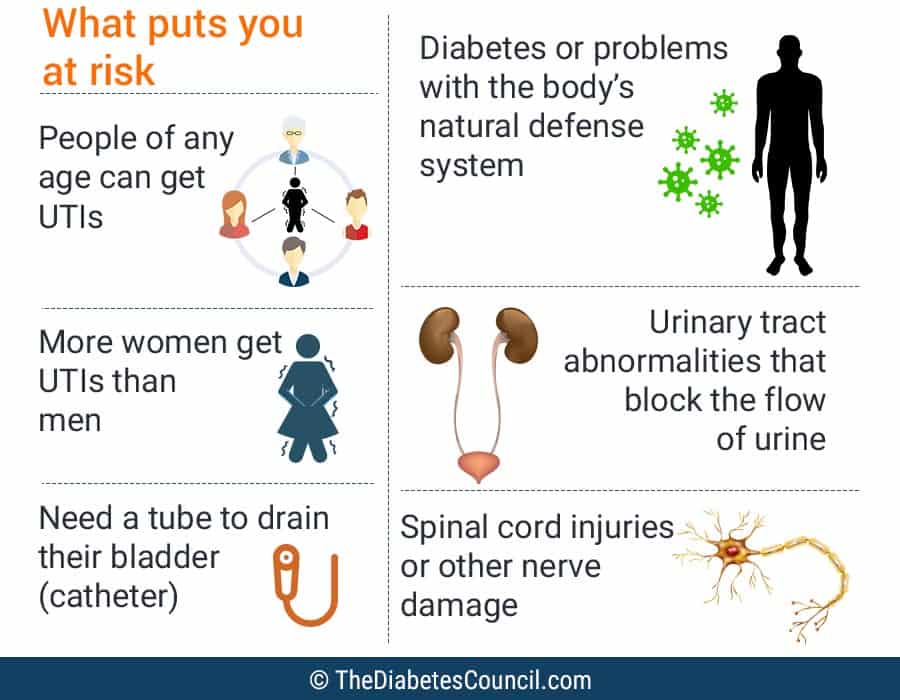
Why does diabetes increase the risk for getting a UTI?
Weaker immune system, poor blood circulation, high blood glucose levels, and diabetic neuropathy (the condition which prevents patients from completely emptying their bladders) are some of the reasons why people with diabetes are at a higher risk
I am a woman, am I at a high risk of getting a UTI?
A study published in the Diabetes Journal by Boyko et al “Diabetes and the Risk of Acute Urinary Tract Infection Among Postmenopausal Women” strong indicates that postmenopausal women are at a higher risk of getting acute symptomatic UTI, especially women who are undergoing treatment for their diabetes. Similarly, a different study confirms that women are 10 times more likely to get one because of their anatomy. Please read above to learn more about this.
What are the signs and symptoms that I should watch for?
The most common signs and symptoms to look out for are:
- Pain and burning during urination
- Not urinating enough
- The urge to urinate more frequently than usual
- Back or abdominal cramps
- Smelly or cloudy urine
- In some extreme cases, watch out for high fever and chills, nausea, vomiting, diarrhea
How can I prevent from getting UTIs on a frequent basis?
Drink a lot of water, check your blood sugar levels frequently, women should be urinating right after intercourse, wiping their bottom from front to back (to prevent germs from the anus reach the urethra), not holding your urine and emptying as necessary.
Further reading:
When should I consider seeing a doctor for my frequent UTIs?
You should see your doctor each time you suspect a UTI. However, please raise your concerns if you are experiencing nausea and vomiting, fever and chills, extremely unusual pain on the lower belly. Ask your doctor to conduct tests to rule out other complications due to diabetes. Don't be embarrassed of such issues and make sure to contact your doctor.
TheDiabetesCouncil Article | Reviewed by Dr. Christine Traxler MD on May 26, 2020
References
- http://www.mayoclinic.org/diseases-conditions/urinary-tract-infection/basics/symptoms/con-20037892
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4346284/#b47-dmso-8-129
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4346284/
- https://www.thediabetescouncil.com/recently-diagnosed-type-1-diabetes-patient-where-do-i-begin/
- https://www.thediabetescouncil.com/type-2-diabetes-an-overview/
- http://care.diabetesjournals.org/content/28/1/177
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3712373/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4346284/
- http://uti.stanford.edu/research/obstructive-urosepsis.html